Chemo Complications, ICU Stay, and Next Steps
In the last update, Bea had just moved forward with her second round of high-dose chemotherapy and stem cell rescue. Shortly after that second transplant, she began having trouble breathing. What initially looked like pneumonia quickly escalated into something much more serious, as she started desatting to ~65% without an oxygen mask. Her lungs became severely inflamed and filled with fluid, and she was diagnosed with ARDS — acute respiratory distress syndrome — a condition where the lungs become too injured to efficiently move oxygen into the bloodstream.
She was transferred to the ICU, where the team could monitor her breathing minute-by-minute, and ultimately decided she needed to be intubated and placed on a ventilator so the machine could do the work of breathing for her while her lungs rested.
A bronchoscopy later showed evidence of diffuse alveolar hemorrhage, which means there had been bleeding deep inside the tiny air sacs of the lungs. This can sometimes happen after high-dose chemotherapy and stem cell transplant, when the lungs are vulnerable.
After 2 weeks on the ventilator, the team attempted an extubation. We hoped her lungs were ready, but they weren’t yet. Even on bipap, she struggled to oxygenate and had to be re-intubated, which was heartbreaking in the moment, but it ultimately gave her lungs the additional time they needed to recover.
Slowly, with steroids and careful respiratory support, the bleeding in her lungs began to settle and the inflammation started to improve. After about another week, they successfully extubated her.
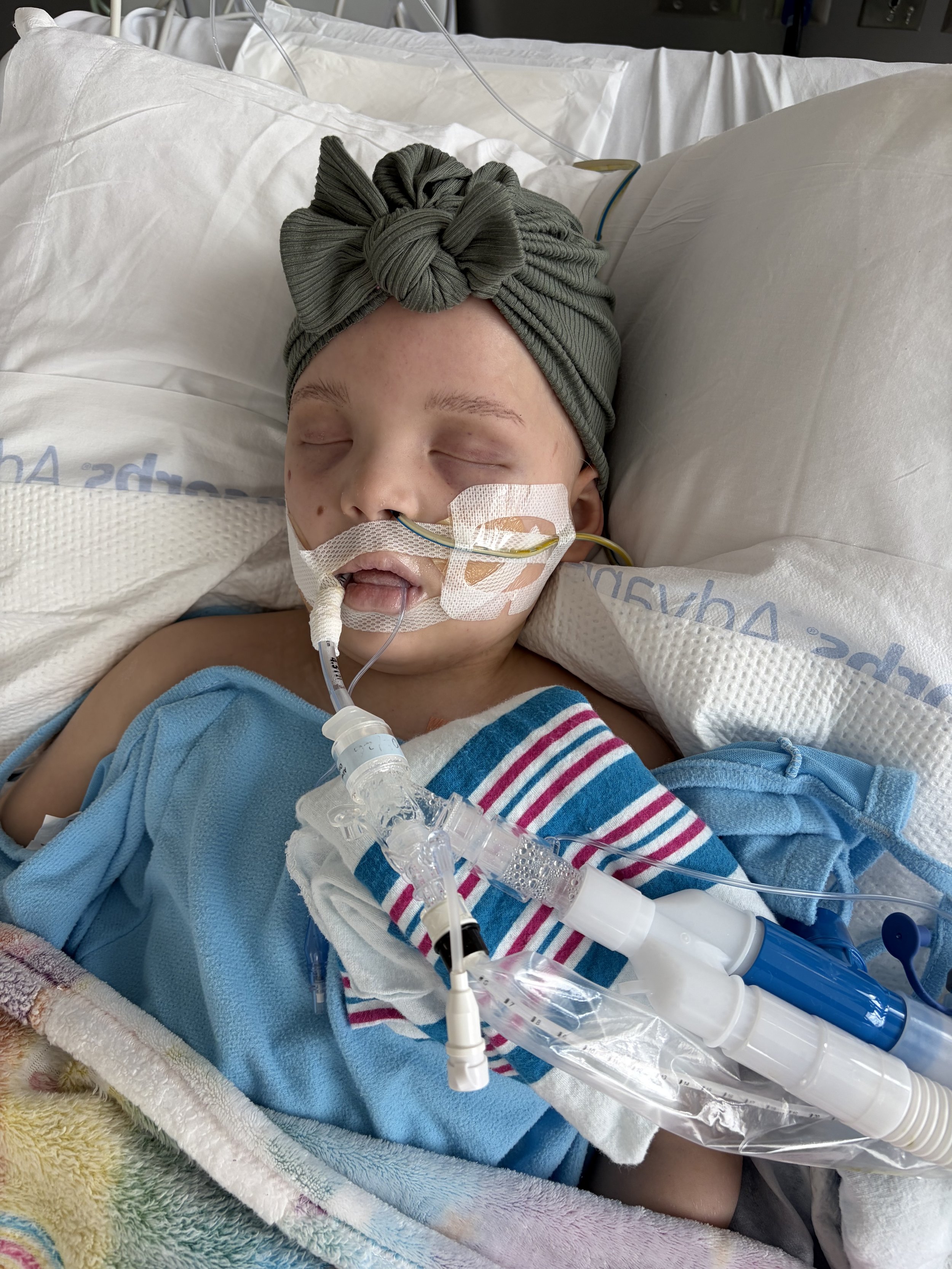
She is now breathing on her own again, with support from alternating BiPAP and high-flow oxygen to help her lungs continue to heal while still giving her body the rest it needs. While she’s very weak from being intubated for so long, and not quite strong enough to talk yet, seeing her awake and breathing on her own has been an enormous milestone.
Because of the severity of what her lungs went through, the team made the thoughtful decision that Bea’s body has been through enough chemotherapy. We will not move forward with the third and final round of high-dose chemo that had originally been planned.
Instead, the focus now shifts to the next and final phase of her treatment: 6 weeks of daily focal proton radiation, targeted to the area in her right frontal lobe where her tumor was originally located.
We had been planning on doing this treatment out-patient at the New York Proton Center, but given everything Bea has been through and the ongoing respiratory support she still needs, the team recommended that this phase happen inpatient at the Children's Hospital of Philadelphia (CHOP), where they can safely deliver proton therapy while continuing to support her recovery.
So our next step will be transferring to Philadelphia once she is stable enough to travel.
The road ahead is still long. Radiation will be another chapter, and recovery from everything her lungs and body went through will take time. But right now we are focusing on the progress in front of us: Bea breathing on her own, healing day by day, and moving toward the final phase of treatment.
With love,
Shannon & Brooks